Magic mushrooms and longevity (new studies)
Contextualizing new studies that point to lifespan and healthspan extending properties of psilocybin mushrooms
People have been asking me about magic mushrooms and Alzheimer’s treatment for a few years now and at first I was admittedly pretty skeptical. People with Alzheimer’s sometimes experience hallucinations and disorientation, which is not helpful for them or their care givers. Giving them a drug that could make that worse seemed to me like a pretty bad idea.
About four years ago, I was looking at the data that was coming out of our platform of genes that relate to slow-brain aging and lo and behold, one of the brain receptors (5-HT2A receptor) that psilocybin mushrooms act upon, was pretty close to the top of that list. This was a piece of our own evidence that magic mushrooms, or other drugs that work through that receptor, might increase health of the brain.
That’s when I started to pay attention.
This past week a study came out in Nature Aging, which showed a 30% lifespan extension in aged mice given psilocybin.
Additionally, a few months ago a small study showed decreased symptoms in people with Parkinson’s disease who had just one dose of magic mushrooms.
Prior to the last few months, there have been >150 ongoing or completed clinical studies of psilocybin for mental health (depression, anxiety) in humans with pretty positive results.
So while I wouldn’t say that I’m convinced— I’m a scientist after all and that bar is pretty high— I would say that I’m feeling pretty optimistic about the potential of psilocybin or analogue drugs to improve brain health or even extend lifespan.
Should we all be taking psilocybin mushrooms? If so, what dose and how often? Are there versions of psilocybin drugs that retain the health benefits without the hallucinations?
First, let’s take a look at the evidence for psilocybin and longevity.
Psilocybin extends lifespan in mice
In a brief communication in Nature Aging from Professor Louise Hecker’s lab at Emory University from just a few days ago, we have the first evidence for psilocybin extending lifespan in mice. While most studies of psilocybin have focused on rejuvenating effects in the brain, this paper focus on the “psilocybin-telomere hypothesis”, which explains psilocybin’s effects on lifespan through its ability to extend telomeres.
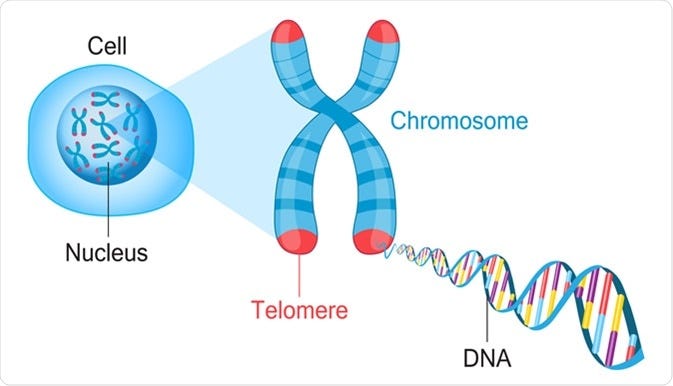
Telomeres are the caps at the end of strands of DNA that get shorter with each new cell division throughout life, eventually becoming so short that cell division no longer works properly and you have a limited ability to replace your blood cells, skin cells, or other cells that need to be frequently replaced.
It’s not necessary for this hypothesis to be true for psilocybin’s lifespan extension in humans since reducing risk of Alzheimer’s (a leading cause of death in older adults) or depression (a leading contributor to death in adults) would in of itself extend lifespan.
To test their hypothesis, the authors started off by treating human lung cells with psilocin (the active metabolite of psilocybin). They showed that psilocin preserved telomere length to a youthful level. It also increased the amount of the putative longevity genes, Sirt1 and NRF2.
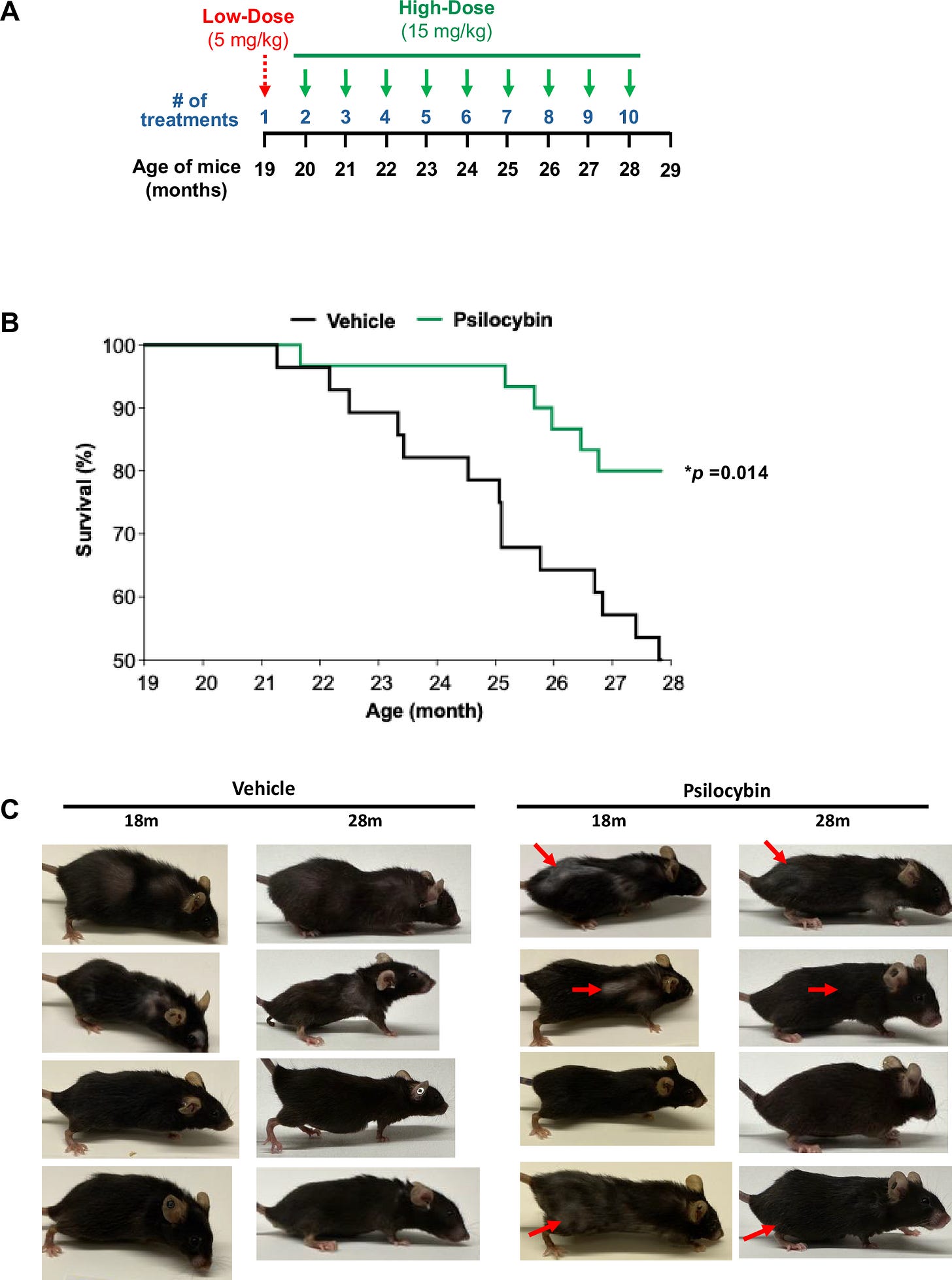
They then treated 19 month old mice (equivalent of 60-65 year old humans) with psilocybin 1X/month for 10 months. The dose that they used in mice was modeled based on a clinical trial in patients, where no serious adverse events were reported at the study endpoint.
The psilocybin treated mice demonstrated significantly higher survival (80%) compared to the control group (50%).
They also mention that the psilocybin-treated mice showed improvements in fur quality, including hair growth and reductions in white hair compared to control mice, although they didn’t quantify this so we don’t know whether it is statistically significant.
A question that I and others have pointed out in this study is why didn’t they follow the psilocybin mice out further to the point where they all die (Figure B)? To see maximum lifespan extension, they would have needed to do this.
Were they just in a rush to get this published?
Also, why didn’t they quantify the fur quality improvements?
In this brief communication, the authors don’t comment on these questions.
Replication of these results will be helpful to flesh out the maximum lifespan extension and whether the fur quality improvements (less grey hair anyone?) are significant.
Psilocybin improves memory in Parkinson’s patients
A study from Professor Ellen Bradley and Professor Joshua Woolley at UCSF’s Translation Psychedelics Research Program in April this year showed improved memory and mood in 12 Parkinson’s patients treated with two doses of psilocybin.
Notably, there was no control group in this pilot study. We know from clients at NeuroAge that it is possible to improve on the PAL test with practice. The PAL test is called Word Pairs in NeuroGames. This means that a study with a control group is necessary to have confidence in these results.
What about other clinical trial data?
Depression and anxiety: A meta-analysis of clinical trial data for psilocybin-assisted treatment of major depression, showed significant benefits in people. Although there were only 436 total participants across the 9 clinical trials and all had “moderate risk of bias”. Many of the studies showed positive benefit for anxiety as well.
Addiction: A review showed positive benefits in 4/4 small clinical studies for alcohol or tobacco use disorders.
Alzheimer’s: There have been no clinical trials for psilocybin for Alzheimer’s treatment to my knowledge. This review summarizes why psilocybin might be helpful in Alzheimer’s with many caveats about ethics. It may be helpful to create a drug that targets the 5HT-2A receptor that doesn’t cause hallucinations for Alzheimer’s.
So we think drugs that target the 5HT-2A receptor might be a good idea for brain health and longevity. Is anyone creating a version that does not cause hallucinations?
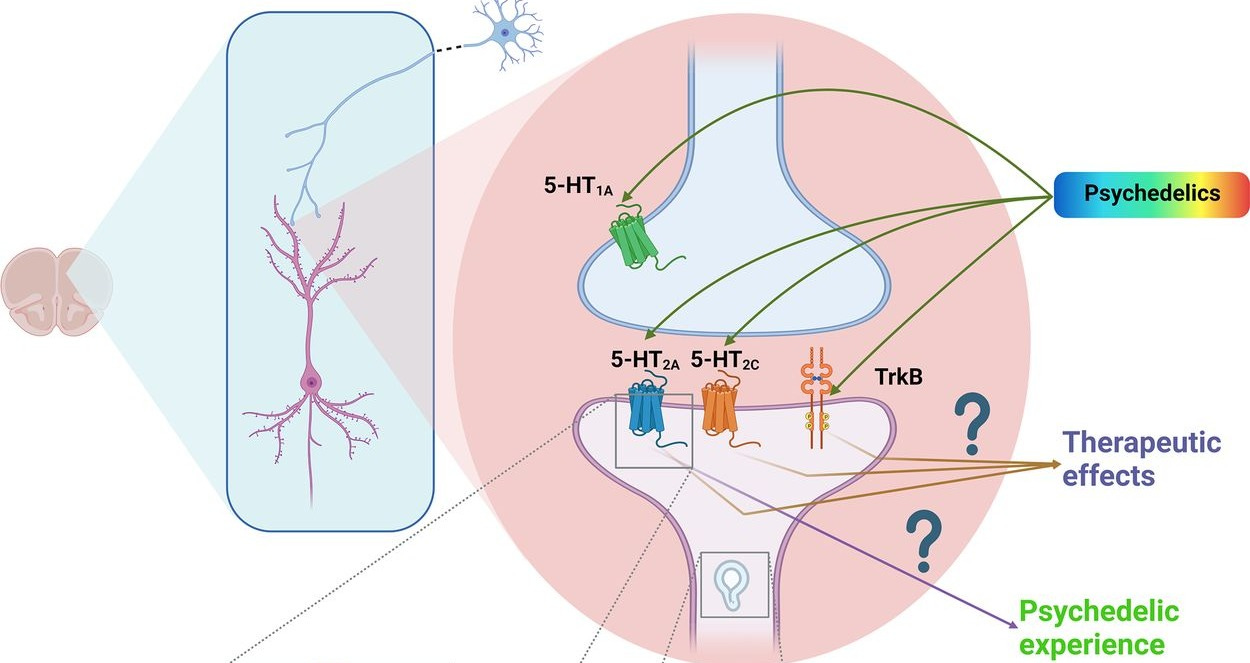
Psilocybin (and other hallucinogens including LSD) also affect other receptors, including the 5-HT1A receptor, the 5-HT2C receptor, and the TrkB receptor (notable because this is the receptor for BDNF (known to be good for the brain). Psilocybin’s affects on those receptors do not cause hallucinations.

Therefore, maybe we can just target the other receptors and get the benefits without the hallucinations?
One piece of counter evidence comes from the NeuroAge platform where we specifically see 5-HT2A and not the other receptors being a top hit for reversing brain aging. This argues for 5-HT2A being necessary.
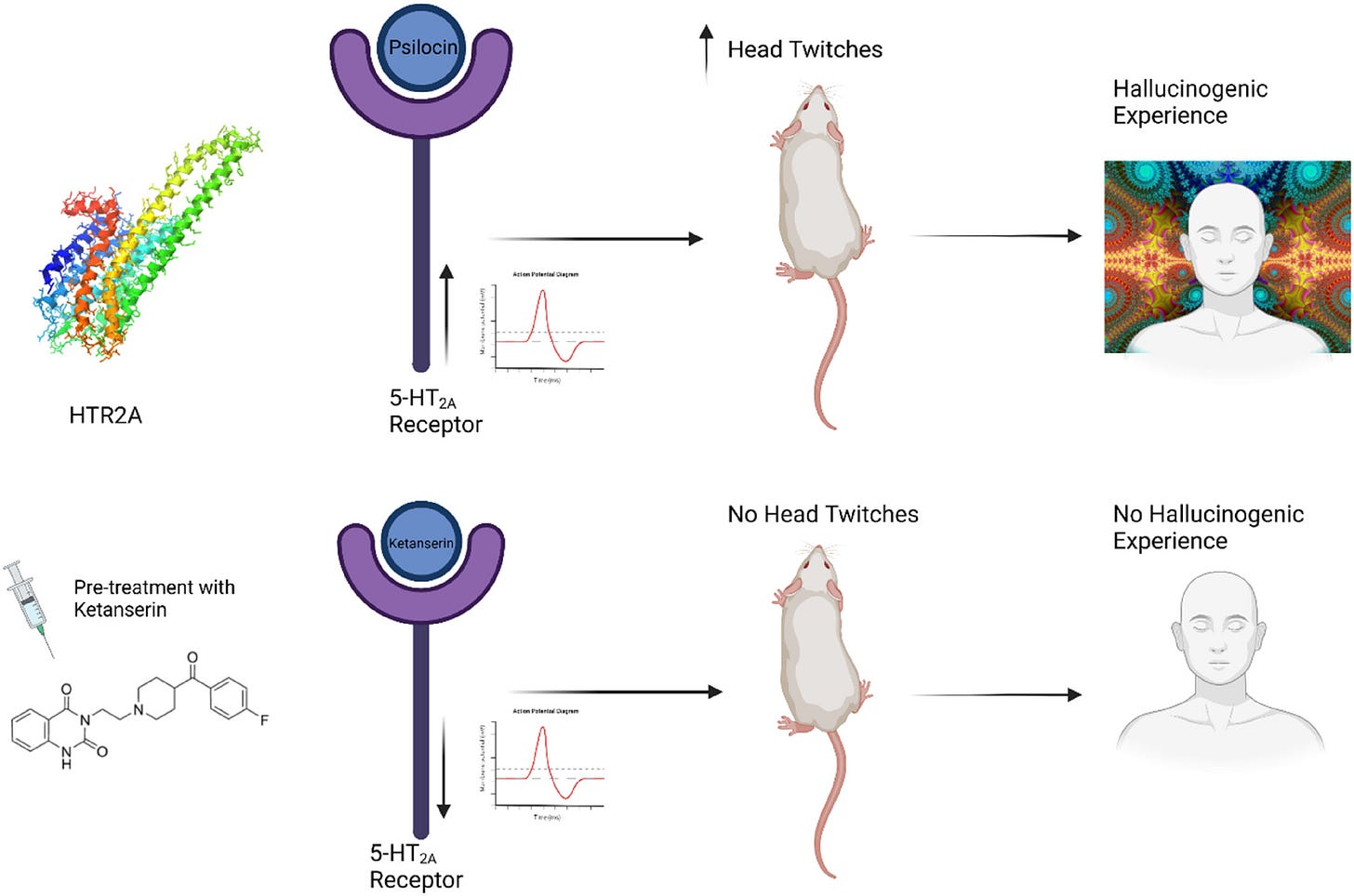
Scientists have tried to tease apart psilocybin’s effects on the 5-HT2A from the other receptors by blocking the ability of psilocybin to bind to 5-HT2A receptor using the antagonist, Ketanserin. Ketanserin also binds to the 5-HT2A receptor but without activating it and blocks the space where psilocybin would bind. Therefore all the effects of psilocybin would go through the other receptors it binds to (see schematic below).
The results of these experiments are mixed and not yet conclusive. They are reviewed here.
That review also discusses several non-hallucinogenic drugs that target the 5HT-2A receptor that are on the market, in clinical trials, or in animal testing. Notably, Lisuride is on the market as a Parkinson’s treatment and works partially through the 5HT-2A receptor but also through dopamine pathways.
2-Br-LSD is a partial 5-HT2A agonist that enhances brain neuroplasticity and promotes the reversal of depression-like behavior in mice but lacks hallucinogenic effects.
So you might want to try psilocybin for health benefits. What’s the right dose?
Clinical trial evidence is reviewed here and excerpted below:
”Both single-dose and two-dose psilocybin treatments significantly reduced depressive symptoms severity, with two-dose administration sometimes yielding more pronounced and lasting effects. However, it is unclear if this was solely due to dosage or other factors. Future research should include standardized trials comparing these dosing strategies to better inform clinical practice.”
What about microdosing?
I know some people that are taking small doses of psilocybin or LSD daily for health benefits. What’s the evidence for this?
Microdosing benefits are unclear. Some argue that the effects are placebo but we don’t have enough evidence to conclude that yet. Microdosing clinical experiments are reviewed here.
In sum, if you are in a place where it is legal and you don’t have health problems that are contraindications, taking a regular dose of psilocybin (2 grams) every month or two has the most evidence for efficacy.
*This post should not be taken as medical advice. Consult your doctor (and your local laws) for any questions regarding psilocybin use.
Summary
In summary, there is mounting, though early, evidence that psilocybin (and potentially other psychedelics) can lessen depression, anxiety, addiction, improve cognition, and even extend lifespan. This could be through their action on the 5HT-2A receptor or other receptors in the brain or telomere lengthening.
Researchers are working on non-hallucinogenic forms of these drugs that may be available in the future. If you’d like to try psilocybin yourself (and you live in a location where it is legal), taking a standard dose every 1-2 months has the most evidence for health benefits.

Written by
Dr. Christin Glorioso, MD PhD
Dr. Glorioso is the founder and CEO of NeuroAge Therapeutics. With her background in neuroscience and medicine, she is dedicated to revolutionizing brain health and helping people maintain cognitive vitality.
Learn more about Dr. Glorioso