Low-Dose Lithium for Brain Health?
Addressing one of the questions people most frequently ask me
Anyone familiar with Dr. Kay Redfield Jamison’s 1995 memoir, An Unquiet Mind, knows the complicated relationship between lithium and cognition. Dr. Jamison, a Johns Hopkins psychiatrist with bipolar disorder, describes cognitive dulling, slowed thinking, memory problems, and emotional blunting at the therapeutic doses (0.6-1.2 mEq/L serum levels) required for mood stabilization. Her account represents a common experience at psychiatric doses. The research discussed in this article involves sub-therapeutic doses (0.25-0.5 mEq/L) that are 2-4 times lower, or microdoses that are roughly 1,000 times lower. The side effect profiles at these reduced levels appear substantially different, though head-to-head comparisons are limited.
For decades, lithium has been a mainstay treatment for bipolar disorder, prescribed at doses that require careful monitoring due to toxicity concerns. Whether much lower doses might protect against cognitive decline remains an open question. Small clinical trials in MCI patients have shown promising results, but the most comprehensive meta-analysis to date found no significant benefit from conventional lithium formulations. Earlier enthusiasm based on ecological studies linking lithium in drinking water to lower dementia rates has been tempered by findings that these associations disappear after adjusting for confounders like obesity and diabetes. A landmark 2025 study from Harvard published in Nature has reignited interest by demonstrating that lithium is naturally present in healthy brains, that its depletion may be among the earliest events in Alzheimer’s pathology, and that a different lithium formulation (orotate) shows efficacy in mice.
The Harvard Discovery
The study by Dr. Aron et al. represents the first demonstration that lithium exists naturally in the human brain and that its loss correlates with cognitive decline. The researchers analyzed postmortem brain tissue from participants in the Rush Memory and Aging Project, measuring trace levels of 27 different metals in people across the cognitive spectrum from healthy to mild cognitive impairment (MCI) to Alzheimer’s disease.
Lithium was the only metal that differed significantly between groups. Levels were high in cognitively healthy individuals but substantially reduced in those with MCI or Alzheimer’s. The researchers discovered that amyloid plaques were sequestering lithium, binding the element and reducing its availability for normal brain functions. In non-plaque regions of affected brains, lithium concentrations correlated with cognitive test scores, suggesting that bioavailable lithium supports cognitive function.
When the team fed mice a lithium-deficient diet, the animals developed increased amyloid deposition, elevated phosphorylated tau, neuro-inflammation, and cognitive deficits. Most intriguingly, supplementation with lithium orotate at approximately 1/1000th of psychiatric doses prevented amyloid accumulation and reversed memory deficits in mouse models of Alzheimer’s disease. Standard lithium carbonate, the formulation used to treat bipolar disorder, proved largely ineffective because it was sequestered by amyloid plaques just as endogenous lithium had been.
Mechanisms of Neuroprotection
Lithium acts on multiple pathways relevant to brain aging and neurodegeneration. The most studied mechanism involves inhibition of glycogen synthase kinase-3β (GSK-3β), an enzyme that phosphorylates tau protein. Elevated phospho-tau is a hallmark of Alzheimer’s pathology, and lithium’s ability to reduce tau phosphorylation at concentrations as low as 0.2 mEq/L has been demonstrated in both cell culture and human cerebrospinal fluid studies.
Beyond GSK-3β inhibition, lithium induces autophagy through an mTOR-independent pathway, potentially enhancing clearance of misfolded proteins including amyloid-β. Studies have shown that lithium increases brain-derived neurotrophic factor (BDNF) expression by several-fold in cortical neurons, supporting synaptic plasticity and neuronal survival. The element also suppresses microglial activation and reduces pro-inflammatory cytokines such as IL-6 and TNF-α, addressing the neuroinflammatory component of Alzheimer’s pathology.
Why Lithium May Blunt Rather Than Sharpen Cognition
A separate mechanism may cut in the opposite direction. Lithium (Li) sits next to sodium (Na) on the periodic table, and this chemical similarity has biological consequences.
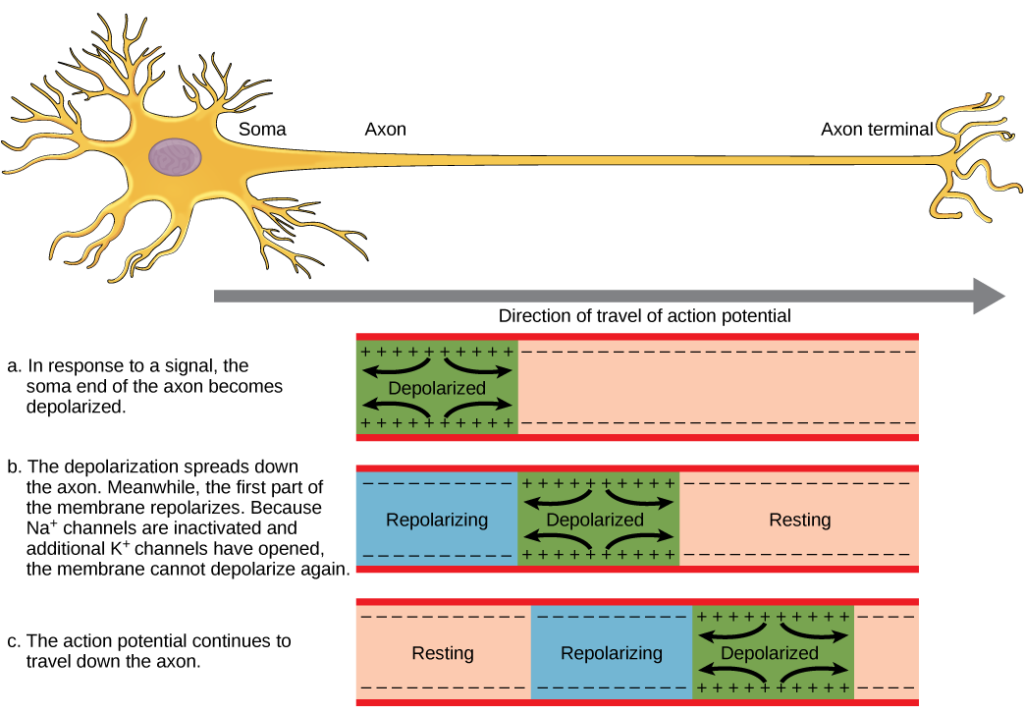
Neurons “fire” or send electrical signals to one another by using charged elements to produce chemical gradients. Specifically sodium (Na+) potassium (K+) pumps maintain a charged gradient that moves down axons (neuron’s cords or cables that connect to other neurons).
Lithium ions can act like sodium and enter neurons through voltage-gated sodium channels, permeating these channels nearly as efficiently as sodium itself. Once inside, lithium displaces intracellular sodium on a one-to-one basis, reducing intracellular sodium concentrations and dampening the electrochemical gradient that drives neuronal firing.
This mechanism helps explain both lithium’s therapeutic effects in mania and the cognitive side effects that Dr. Jamison and others describe at psychiatric doses. Hyperactive neurons fire more frequently, opening their sodium channels more often and allowing more lithium to accumulate inside. The result is preferential dampening of overactive circuits. But at therapeutic doses, this effect is not selective enough to spare normal cognition. The same sodium displacement that calms manic episodes also slows processing speed, blunts emotional responsiveness, and impairs memory.
To put it simply, Lithium stops neuronal firing. All firing, not just the unwanted overactive firing in mania. It’s a sledge hammer.
The critical question for low-dose supplementation is whether sub-therapeutic lithium levels can deliver neuroprotective benefits (via GSK-3β inhibition and autophagy) without meaningfully reducing neuronal excitability. This remains unproven. If the clinical trial data showing cognitive benefits prove unreliable (see recent negative meta-analyses in the next sections), what remains is a compound whose primary mechanism of action is to reduce neuronal firing. For a cognitively healthy person without pathological processes to counteract, this could mean subtle cognitive dulling rather than enhancement. The sodium channel mechanism suggests that lithium is mechanistically the opposite of a nootropic, and any cognitive benefits would need to come from other pathways overwhelming this baseline effect.
Evidence from Clinical Trials
Nine randomized controlled trials have examined lithium for cognitive outcomes in MCI or Alzheimer’s disease. The pattern that emerges is consistent. Trials lasting 12-24 months in MCI patients using sub-therapeutic doses show benefit, while short trials (10 weeks) or those in established Alzheimer’s disease generally do not. The two largest and longest trials, both targeting MCI with low-dose lithium carbonate over two years, found statistically significant slowing of cognitive decline. Please note that the Harvard study was with lithium orotate, a different formulation, and the researchers saw no benefits of lithium carbonate in the mouse studies. Side effects of lithium carbonate at these doses include diarrhea, fatigue, and tremor in roughly 15-30% of participants above placebo rates, but serious adverse events were not attributable to the medication and no significant deterioration in kidney or thyroid function occurred over up to four years of follow-up.
How meaningful are these effects, and should we trust them? Dr. Matsunaga’s 2015 meta-analysis found a standardized mean difference (SMD) of -0.41, which falls in the medium effect size range. But Dr. Kishi’s 2025 meta-analysis found no significant effect at all, calling into question whether the earlier positive findings were robust. The individual positive trials (Forlenza, LATTICE) showed real benefits, but with only 61-80 participants each, they may have been underpowered to detect true effect sizes or may have benefited from chance.
For context on what a real effect would mean if it exists, consider comparisons to approved treatments. The FDA-approved anti-amyloid antibodies lecanemab and donanemab show small effect sizes (Cohen’s d of 0.21 and 0.26 respectively) on the CDR-SB scale, and their absolute benefits of 0.45-0.70 points fall below the threshold of 1.0 point considered the minimal clinically important difference for MCI patients. Cholinesterase inhibitors like donepezil produce larger absolute improvements on cognitive scales (roughly 2.7 points on the 70-point ADAS-Cog), but these are symptomatic effects that do not modify disease progression and tend to wane over time.
Exercise provides another comparator. Meta-analyses of physical activity interventions in MCI find effect sizes ranging from 0.30 for general physical exercise to 0.54-0.76 for aerobic exercise and up to 1.05 for resistance training. The positive lithium trials’ effect sizes fall in this range, comparable to moderate aerobic training. The Forlenza trial’s 50% reduction in dementia conversion (16% versus 30% over four years), while not statistically significant due to small sample size, would represent a meaningful clinical benefit if it holds in larger trials. But absent replication in adequately powered studies, these remain preliminary findings.
The strongest human evidence for low-dose lithium’s cognitive benefits comes from a series of trials conducted by Dr. Forlenza and colleagues in São Paulo, Brazil. Their 2011 study randomized 45 older adults with amnestic MCI to receive lithium carbonate at subtherapeutic doses (targeting serum levels of 0.25-0.5 mEq/L, compared to 0.6-1.2 mEq/L for psychiatric treatment) or placebo for 12 months. Lithium treatment was associated with a significant reduction in cerebrospinal fluid phosphorylated tau.
The 2019 follow-up extended observation to 24 months with an additional 24-month open-label extension, enrolling 61 participants total. Participants receiving lithium remained cognitively stable over two years while those on placebo showed continuous decline, with the lithium group performing better on memory and attention tests. At four years, 16% of lithium-treated patients had converted to dementia compared to 30% of placebo patients, a nearly 50% relative risk reduction that approached statistical significance (p=0.06).
A 13-year follow-up evaluation published in 2023 found that those originally randomized to lithium maintained better global cognitive outcomes than matched controls who never received the intervention. This remarkable durability of effect suggests that lithium may genuinely modify the disease course rather than merely providing symptomatic benefit.
The recently completed LATTICE trial from the University of Pittsburgh replicated these findings in 80 American participants with MCI. Over two years, verbal memory (measured by the CVLT-II) declined by 0.73 points annually in the lithium group compared to 1.42 points in the placebo group, a statistically significant difference (p=0.048). While most secondary outcomes did not reach significance, the trial’s primary finding confirmed that subtherapeutic lithium carbonate slows verbal memory decline in MCI.
Not all trials have been positive. A 10-week German trial in patients with established Alzheimer’s disease found no effect on cognition or biomarkers, but this short duration was likely insufficient to observe neuroprotective benefits. The pattern across studies suggests that lithium requires months to years of exposure to manifest its effects and works better in early disease stages when neuronal damage is still reversible.
Meta-Analyses Present a Mixed Picture
The most recent and comprehensive synthesis of the evidence is sobering. A 2025 meta-analysis by Dr. Kishi et al., incorporating six trials and 435 participants, found no significant overall benefit from conventional lithium salts on cognitive function in MCI or Alzheimer’s disease. This included lithium carbonate, gluconate, and sulfate formulations.
An earlier 2015 meta-analysis by Dr. Matsunaga et al. had pooled three trials comprising 232 participants and found that lithium significantly decreased cognitive decline compared to placebo with a medium effect size (SMD -0.41, p=0.04). The discrepancy between these analyses likely reflects the inclusion of additional negative trials in the 2025 analysis and highlights how sensitive pooled results are to study selection.
The apparent disconnect between positive individual trials and negative meta-analyses may also reflect formulation differences. All human trials to date have used lithium carbonate, lithium sulfate, or lithium gluconate. If the Harvard findings hold, these conventional salts are suboptimal because they are sequestered by amyloid plaques, leaving little lithium available to protect neurons. Lithium orotate, which appears to evade amyloid binding in mouse studies, has never been tested in a controlled human trial despite being widely available as an over-the-counter supplement.
Ecological Evidence from Drinking Water
Trace amounts of lithium occur naturally in drinking water at concentrations far below therapeutic levels, typically ranging from less than 1 μg/L to over 50 μg/L depending on local geology. A 2017 Danish study published in JAMA Psychiatry examined over 800,000 people and found that exposure to drinking water containing more than 15 μg/L of lithium was associated with a 17% lower incidence of dementia compared to the lowest exposure category. The relationship was non-linear, with intermediate levels (5.1-10 μg/L) paradoxically associated with slightly increased risk before protection emerged at higher concentrations.
However, subsequent studies have raised doubts about these findings. Research from Texas and other U.S. regions initially showed similar protective associations, but these effects disappeared after adjusting for obesity, diabetes, and physical activity. This suggests that the Danish results may reflect confounding by metabolic health factors or other regional characteristics rather than a true lithium effect. A Scottish study found no protective effect, though the lithium levels in Scottish drinking water (0.1-9.2 μg/L) were below the apparent threshold suggested by the Danish data. The ecological evidence, while hypothesis-generating, cannot establish causation and may be explained by factors unrelated to lithium.
Safety at Low Doses
The side effects that make psychiatric-dose lithium challenging to use, including tremor, polyuria, weight gain, and thyroid dysfunction, appear to be largely dose-dependent and minimal at subtherapeutic levels.
The LATTICE trial provides the most detailed recent safety data at low doses. Serious adverse events occurred in 29% of lithium-treated participants compared to 23% on placebo, but none were definitively attributed to the study medication. The most common side effects were diarrhea (29% vs 15% on placebo), fatigue (29% vs 15%), and tremor (24% vs 15%). Notably, creatinine elevations occurred at similar rates in both groups (29% vs 31%), suggesting that low-dose lithium does not meaningfully affect kidney function.
The Forlenza trials followed participants for up to four years and found no significant deterioration in renal function, thyroid parameters, immune markers, or glucose metabolism. One secondary imaging analysis raised the possibility that lithium might reduce hippocampal volume, which would be concerning given this structure’s vulnerability in Alzheimer’s disease. This finding requires further investigation but has not been replicated.
At microdose levels (300 μg/day, approximately 1/1000th of psychiatric doses), no adverse events have been reported in the limited available data. This dosing approximates what some people obtain naturally from mineral-rich drinking water.
Dosing and Formulations
The gap between clinical trial evidence and practical supplementation presents challenges. The positive MCI trials used lithium carbonate titrated to achieve serum levels of 0.25-0.5 mEq/L, which requires prescription medication and periodic blood monitoring. Over-the-counter lithium orotate supplements typically contain 5 mg of elemental lithium per tablet (from 120 mg of lithium orotate), which is far below the doses used in trials but aligns with the microdose range suggested by the Harvard mouse studies.
Early research suggested that lithium orotate might achieve three-fold higher brain concentrations than carbonate at equivalent doses, potentially allowing lower peripheral levels and reduced side effects. However, no human pharmacokinetic studies have directly compared brain penetration between formulations. The 2025 Harvard findings that orotate evades amyloid sequestration while carbonate does not provide a compelling mechanistic rationale for preferring orotate, but this has not been validated in human trials.
APOE4 and Lithium
For individuals carrying the APOE4 allele, lithium may be particularly relevant. APOE4 carriers experience elevated GSK-3β activity, increased tau phosphorylation, iron dysregulation, and heightened susceptibility to ferroptosis (iron-dependent cell death). A 2025 study using induced pluripotent stem cells from APOE4/E4 individuals found that lithium chloride improved cell viability, reduced cytosolic iron accumulation, restored protective GPX4 levels, and reduced lipid peroxidation. Some longevity medicine practitioners have begun recommending low-dose lithium specifically to APOE4 carriers given this mechanistic rationale, though controlled trials in this population are lacking.
Current Limitations and Future Directions
Despite decades of research, critical questions remain unanswered. No randomized controlled trial has tested lithium orotate in humans with MCI or Alzheimer’s disease, even though this formulation shows the most promise based on preclinical data. Dr. Yankner’s laboratory at Harvard is reportedly planning such a trial. No primary prevention study has examined whether lithium supplementation in cognitively healthy individuals reduces subsequent dementia risk over years or decades. The optimal dose for neuroprotection remains undefined, with evidence ranging from micrograms to milligrams daily.
Dr. Kishi’s 2025 meta-analysis concluded that conventional lithium salts do not significantly improve cognition in MCI or Alzheimer’s disease when pooled across trials. This finding should temper enthusiasm while underscoring the importance of testing alternative formulations. If lithium orotate truly evades amyloid sequestration as the Harvard data suggest, results from carbonate trials may systematically underestimate lithium’s potential.
Practical Considerations
For individuals interested in low-dose lithium supplementation, several considerations apply. Over-the-counter lithium orotate is widely available and provides approximately 5 mg of elemental lithium per standard tablet. This dose approximates dietary intake in regions with lithium-rich drinking water and is far below levels requiring medical monitoring. However, no regulatory body has evaluated lithium orotate supplements for efficacy or safety in dementia prevention.
Those considering higher doses in the subtherapeutic range (such as the 0.25-0.5 mEq/L target used in clinical trials) would require prescription lithium carbonate and medical supervision including periodic assessment of renal and thyroid function. Drug interactions are dose-proportional but present at any level. NSAIDs, ACE inhibitors, ARBs, and thiazide diuretics can all increase lithium levels by 25-40%, and individuals taking these medications should exercise caution.
Where We Stand
The case for low-dose lithium in brain health is intriguing but unproven. The 2025 Harvard discovery that brain lithium depletion may be an early event in Alzheimer’s pathogenesis provides a compelling mechanistic framework. Small clinical trials have shown that sub-therapeutic lithium carbonate may slow cognitive decline in MCI over periods of two to four years. But the most comprehensive meta-analysis found no overall benefit from conventional lithium formulations, no human trial has tested the orotate formulation that showed striking effects in mice, and the ecological associations from drinking water studies appear to be confounded by metabolic health factors.
The gap between preclinical promise and clinical evidence is substantial. Lithium orotate supplements are widely available and inexpensive, yet the formulation has never been tested in a rigorous human trial for cognitive outcomes. The positive individual trials used lithium carbonate at doses requiring medical supervision, not the over-the-counter orotate products that consumers can purchase. And the mouse studies, however elegant, may not translate to humans.
Professor Bruce Yankner, the senior author of the Harvard study, captured the appropriate caution in a recent interview, noting that before recommending lithium orotate to patients, researchers need to determine the effective and safe dose range in people. His laboratory is planning a clinical trial, and the results may clarify whether lithium can meaningfully contribute to preventing or treating Alzheimer’s disease. One secondary imaging analysis raised the possibility that lithium might reduce hippocampal volume, which would be concerning given this structure’s vulnerability in Alzheimer’s disease. Given the negative meta-analysis, the absence of human orotate trials, the ecological associations that disappear after adjusting for metabolic confounders, and the unresolved safety questions, I do not currently recommend low-dose lithium supplementation for brain health.
Also, I read Dr. Jamison’s memoir at the time and frankly, that’s not what I want in my nootropics, handwaving about dosing and formulation not withstanding.

Written by
Dr. Christin Glorioso, MD PhD
Dr. Glorioso is the founder and CEO of NeuroAge Therapeutics. With her background in neuroscience and medicine, she is dedicated to revolutionizing brain health and helping people maintain cognitive vitality.
Learn more about Dr. Glorioso