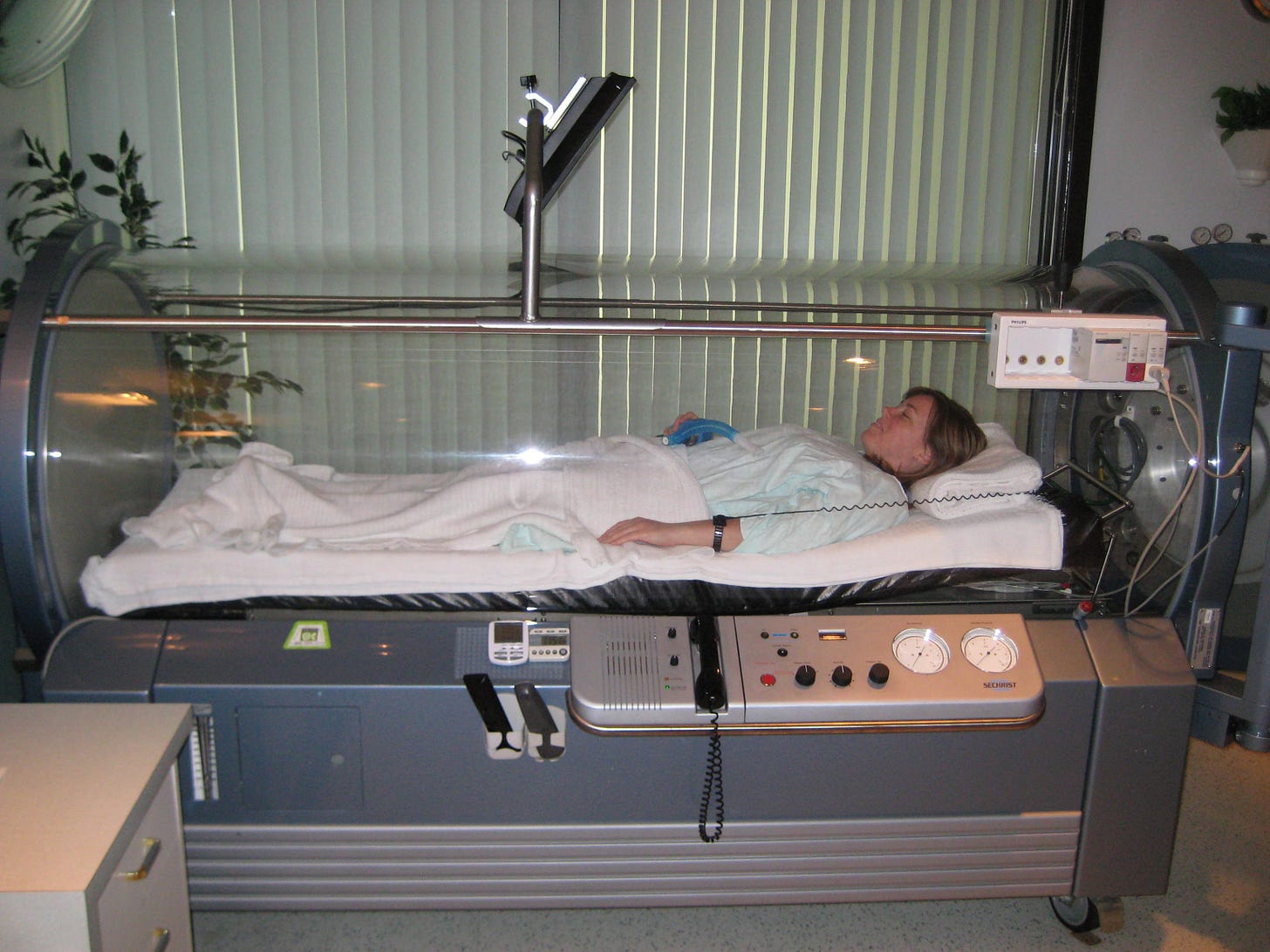
HBOT for Brain Health
What the science tells us and is it worth the time and cost
I'm frequently asked whether Hyperbaric Oxygen Therapy (HBOT) is worth it for dementia prevention and longevity.
I haven’t been motivated to try it myself and this deep dive explains why. At least it explains why not now. Entrepreneurial and engineering advances combined with additional human data could change that calculus for me.
The above picture partially demonstrates why I don’t want to do this. 90 minutes five days a week in that glass box seems like spending time in a coffin or as a body in a morgue to me. While not everyone feels this way I’m sure, that’s how it feels to me.
90 minutes is also a lot of time that I could be spending on other things for my health, like exercise, sleep, healthy cooking, and community. There are only so many hours in the day.
That said, HBOT shows intriguing potential for cognitive enhancement and brain aging reversal through multiple biological mechanisms. And although the evidence in humans is preliminary, it’s promising.
Here I cover how HBOT came to be, the scientific evidence and mechanisms, and the practical aspects of where we need to go for this to be widely adopted.
How HBOT moved from diving medicine to brain health
1662: The first pressurized chamber was built by a British clergyman named Henshaw, who used bellows to compress air for vague health claims. This was over a century before oxygen was even discovered.
1830s: Fashionable “compressed air spas” opened across Europe to treat tuberculosis and other ailments.
1930s-1939: When divers or underwater construction workers ascend too quickly, nitrogen dissolved in their blood forms bubbles, causing joint pain, paralysis, or in severe cases, loss of life. This condition was called “the bends” or decompression sickness. Researchers discovered that putting affected divers back under pressure (recompression) could reverse symptoms, and adding 100% oxygen worked even better. The US Navy adopted HBOT for decompression sickness in 1939.
1970s: The jump to neurological applications came through serendipity. Dr. Richard Neubauer was treating two multiple sclerosis patients with HBOT for chronic bone infections (an approved indication) when he noticed unexpected neurological improvements. This led him to apply HBOT to stroke patients.
1990: Dr. Neubauer published a letter in The Lancet introducing the concept of “idling neurons,” arguing that damaged brain cells were not necessarily gone forever but could be metabolically suppressed and potentially recoverable with oxygen. This challenged the prevailing view in neurology that neurons were simply dead or alive, with nothing to be done for chronic brain injury.
1990s: Dr. Paul Harch in New Orleans noticed that some divers had lingering cognitive problems even after successful acute treatment for decompression sickness. When he treated these chronic cases with additional HBOT, they showed cognitive improvement. He began using SPECT brain imaging to document blood flow changes before and after treatment, providing visual evidence of the therapy’s effects.
2010s: Dr. Shai Efrati’s group at the Sagol Center in Israel began running more rigorous trials on stroke and traumatic brain injury, then extended the research to healthy aging, producing the trials discussed below.
The clinical evidence is strongest for attention and processing speed
The key randomized controlled trial on healthy cognitive aging comes from Dr. Amir Hadanny and colleagues (2020, Aging), which enrolled 63 healthy adults over age 64 and administered 60 daily HBOT sessions at 2.0 ATA with 100% oxygen. The HBOT group showed substantial improvements across cognitive domains, with large effect sizes for global cognition (d=0.85), attention (d=0.75), processing speed (d=0.79), and executive function (d=0.84-0.86). Memory and verbal fluency showed more modest gains (d=0.57-0.59).
Neuroimaging corroborated these findings, demonstrating significant cerebral blood flow increases in prefrontal and parietal regions on perfusion MRI. Moderate correlations (r=0.34-0.45) linked regional blood flow improvements to cognitive gains, providing mechanistic support for the clinical observations.
The same research group documented anti-aging biomarker changes in a related study. Dr. Yafit Hachmo and colleagues (2020, Aging) found that 60 HBOT sessions increased telomere length by over 20% across immune cell populations. Telomeres are the protective caps on chromosome ends that shorten with age. The study also found 37% reductions in senescent T-helper cells. Senescent cells are “zombie cells” that have stopped dividing but remain metabolically active, secreting inflammatory signals that damage surrounding tissue. However, this single-arm study with only 35 participants and no control group requires replication, and whether these biomarker changes translate to functional benefits remains unestablished.
Evidence in MCI and Alzheimer’s disease is limited
Dr. Jianwen Chen and colleagues (2020, Alzheimer’s & Dementia: TRCI) at Dalian Medical University in China treated 11 amnestic MCI patients with 20 HBOT sessions, finding significant MMSE and MoCA improvements at 1-3 month follow-up. (The MMSE and MoCA are standardized cognitive screening tests used to detect memory and thinking problems.) PET imaging in a subset showed improved brain glucose metabolism. However, this was a non-randomized study with a small sample size.
A 2024 meta-analysis (Dr. Guoyu Lin et al., Frontiers in Aging Neuroscience) of 11 randomized trials with 847 Alzheimer’s patients found a mean improvement of 3.08 points on the MMSE, a potentially meaningful effect on a 30-point scale. However, all 11 trials were conducted in China, many combined HBOT with medications like donepezil rather than testing HBOT alone, and methodological quality varied across studies. No trials have examined whether HBOT prevents dementia in at-risk populations.
Biological mechanisms are largely preclinical
HBOT’s potential brain aging effects operate through interconnected molecular pathways. Multiple human imaging studies demonstrate 16-23% cerebral blood flow increases following HBOT through VEGF-driven angiogenesis (VEGF is a protein that stimulates new blood vessel formation). Dr. Ronit Shapira and colleagues (2021, Aging) showed HBOT increased arteriolar luminal diameter in Alzheimer’s mouse models, reducing hypoxia.
The remaining mechanisms are demonstrated primarily in animal models.
1. Neurogenesis and neuroplasticity (animal data, supported by human imaging). Multiple animal studies show HBOT enhances neural stem cell proliferation, hippocampal neurogenesis, and synaptic plasticity through BDNF upregulation. (BDNF, or brain-derived neurotrophic factor, is a protein that supports neuron survival and growth.) Human neuroimaging shows hippocampal structural changes correlating with memory improvements.
2. Mitochondrial biogenesis (animal data). Mitochondria are the energy-producing structures within cells, and their function declines with age. HBOT activates the SIRT-1/PGC-1α/TFAM pathway, which are master regulators of mitochondrial production. Dr. Hung-Te Hsu and colleagues (2022, Biomolecules) demonstrated this in Parkinson’s mouse models.
3. Neuroinflammation reduction (animal data). Dr. Ronit Shapira and colleagues (2018, Neurobiology of Aging) showed HBOT in 3xTg-AD mice (a triple-transgenic Alzheimer’s model) reduced astrogliosis and microgliosis while shifting microglial polarization from pro-inflammatory M1 to anti-inflammatory M2 phenotype.
4. Amyloid and tau reduction (animal data). HBOT reduced pre-existing plaque volume, attenuated new plaque formation, and decreased tau phosphorylation in Alzheimer’s mouse models. Long-term studies (Dr. Chun-Hua Yang et al., 2024, Redox Biology) showed 3-month HBOT reduced both Aβ plaques and hyperphosphorylated tau.
5. Glymphatic system enhancement (theoretical). The glymphatic system is the brain’s waste-clearance network that removes toxic proteins during sleep. HBOT’s effects on this system remain theoretical with no direct studies to date.
6. Oxidative stress modulation (animal data). Following hormetic principles, controlled ROS (reactive oxygen species) elevation activates the Nrf2/ARE pathway, inducing antioxidant genes. Multiple studies show HBO preconditioning increases antioxidant enzyme activity.
The type of HBOT chamber and protocol matters
A critical distinction exists between “mild” HBOT marketed in wellness settings and medical-grade protocols used in research. At home soft chambers have limited evidence for efficacy (1.3 ATA). ATA stands for 'atmospheres absolute,' a measure of pressure where 1.0 ATA is normal sea level pressure and 2.0 ATA is twice that pressure.
Medical-grade hard chambers (2.0-2.8 ATA):
Steel or acrylic construction that can withstand high pressures
Deliver 100% oxygen via mask
At 2.0 ATA with 100% oxygen: 94% increase in oxygen delivery to tissues
Used in all the clinical research on cognitive enhancement
Require trained technicians, located at clinics
Sessions cost $100-250+ for 90 minutes each, with research protocols using 40-60 sessions ($4,000-15,000 total)
90-minute sessions with 5-minute air breaks every 20 minutes to trigger the hyperoxic-hypoxic paradox
Soft chambers (1.3 ATA):
Inflatable fabric construction, limited to lower pressures
Use ambient air (21% oxygen) or oxygen concentrators reaching approximately 30%
At 1.3 ATA with air, there is only a 3% increase in oxygen delivery
No published evidence for cognitive or anti-aging benefits
Can be purchased for home use ($5,000-15,000), but do not reach the pressure or oxygen levels used in any of the cognitive enhancement research
Often marketed as “wellness” devices
The Undersea and Hyperbaric Medical Society states it is not aware of any reliable clinical evidence that mild compression to less than 1.4 ATA has any therapeutic effect.
Standard medical-grade protocols require 40-60 sessions administered daily, 5 days weekly over 2-3 months.
The safety profile is favorable but not without risks
HBOT demonstrates acceptable safety in elderly populations. Pressure injuries to the eardrum affect 9-13% of patients but are typically mild. Temporary nearsightedness occurs in 20-31% of participants, resolving 6-8 weeks post-treatment. Oxygen toxicity causing seizures is rare, occurring roughly once per 2,000-3,000 treatments.
Contraindications include active pneumothorax (collapsed lung), certain chemotherapy agents, severe COPD with air trapping, and claustrophobia. These safety data derive from supervised medical settings and may not apply to unsupervised home use of soft chambers.
The human evidence has methodological limitations
The key healthy aging trial enrolled only 63 participants, and the telomere study had 35. Adequately powered trials (n=300+) are absent from the literature.
Using pressurized room air (1.2-1.3 ATA) as “sham” likely provides some biological activity, confounding interpretation. The Sagol Center in Israel has produced the largest body of work on HBOT and aging. Broader replication across diverse research institutions would strengthen confidence.
Cost and time commitments
Hospital-based programs treat only FDA-approved indications like wound healing and decompression sickness, and will not offer HBOT for cognitive applications. However, independent medical-grade clinics with hard chambers capable of 2.0+ ATA and 100% oxygen exist in most major metropolitan areas and do offer off-label treatment for cognitive and longevity purposes. Sessions run $100-250 each, making a 40-60 session protocol $4,000-15,000 out-of-pocket. Insurance does not cover off-label use.
The path to widespread consumer use
Protocol optimization (the biggest unknown):
The 60-session protocol was tested, not proven optimal. The MCI study used only 20 sessions. Research determining minimum effective dose could dramatically reduce time and cost.
Shorter sessions that achieve similar oxygen saturation
Less frequent sessions (maintenance protocols after initial loading)
Identifying who responds best, so not everyone needs the full protocol
Technology and cost reductions:
Hard chamber manufacturing costs coming down over time
Smaller-footprint hard chambers designed for home installation
Shared equipment models at gyms or wellness centers with multiple medical-grade chambers
Being able to multi-task while doing this would also change things for me. Imagine HBOT being seamless enough to be in Ubers or while sleeping.
Business model innovations:
HBOT facilities with membership access to hard chambers (some are emerging)
Integration into existing fitness and recovery facilities
Regulatory and insurance:
FDA approval for cognitive indications would drive insurance coverage and make clinic treatment financially accessible
Large RCTs showing dementia prevention would change everything
The research that matters most now is dose-response and durability. If 10 sessions maintains benefits for a few years, the calculus changes entirely.
In Summary
For cognitive enhancement in healthy older adults, small trials show improvements in attention, processing speed, and cerebral blood flow with large effect sizes. The key trial used 60 sessions at 2.0 ATA with 100% oxygen over 3 months, though the MCI study saw improvements with only 20 sessions. The minimum effective dose is unknown. Effects were measured at end of treatment, with no published long-term follow-up showing how long benefits persist. Evidence in MCI and Alzheimer’s disease is weaker and no trials have examined dementia prevention. Animal studies demonstrate multiple plausible mechanisms including reduced neuroinflammation, improved mitochondrial function, and decreased amyloid and tau accumulation.
For those who want to try HBOT, independent medical-grade clinics with hard chambers exist in most major metropolitan areas and offer off-label treatment at $100-250 per session. Home soft chambers at 1.3 ATA with air do not reach the protocols used in research and lack evidence of cognitive benefit.
For those inclined to wait, the key research to watch is dose-response and durability studies. If fewer sessions or periodic maintenance protocols prove effective, and if effective at home options or “HBOT-Uber” options emerge, HBOT could become a more practical option for brain health.

Written by
Dr. Christin Glorioso, MD PhD
Dr. Glorioso is the founder and CEO of NeuroAge Therapeutics. With her background in neuroscience and medicine, she is dedicated to revolutionizing brain health and helping people maintain cognitive vitality.
Learn more about Dr. Glorioso